Brain cells, which lack regenerative capacity, must be very well protected. The system called the blood–brain barrier assumes this role. By preventing harmful compounds and microorganisms from passing from the blood into the brain while regulating the supply of nutrients to the brain, this barrier is a multifunctional miraculous system. Functioning almost like a strict customs gate, it protects the central nervous system—composed of the brain and spinal cord—through its meticulousness and high selectivity.
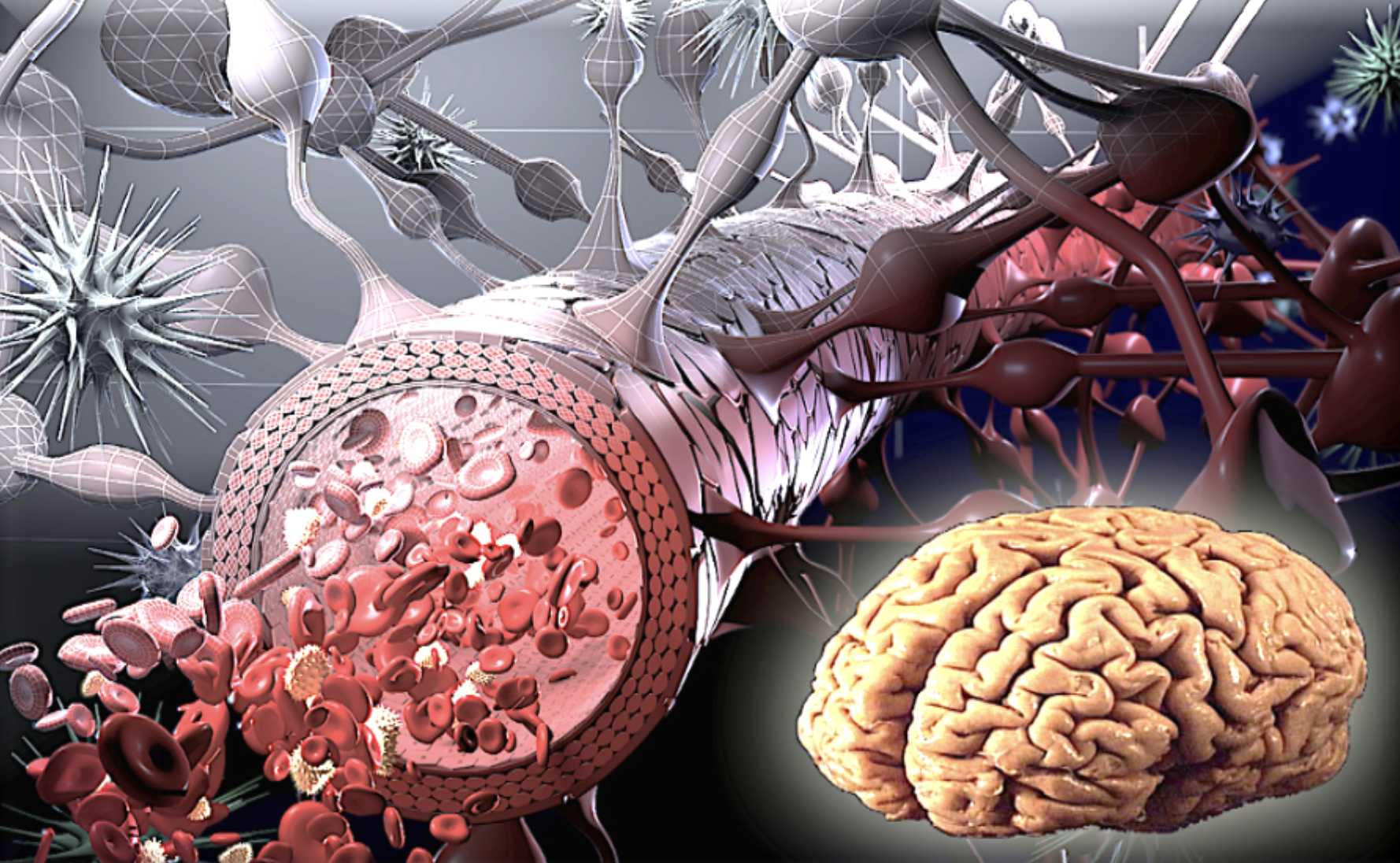
The terminal capillaries in extremities distant from the main center, such as the arms and legs, allow many substances to pass into cells. However, by means of the special structure of the blood–brain barrier, the passage of substances into brain cells is tightly controlled. Both physical and metabolic factors play a role in this restriction.
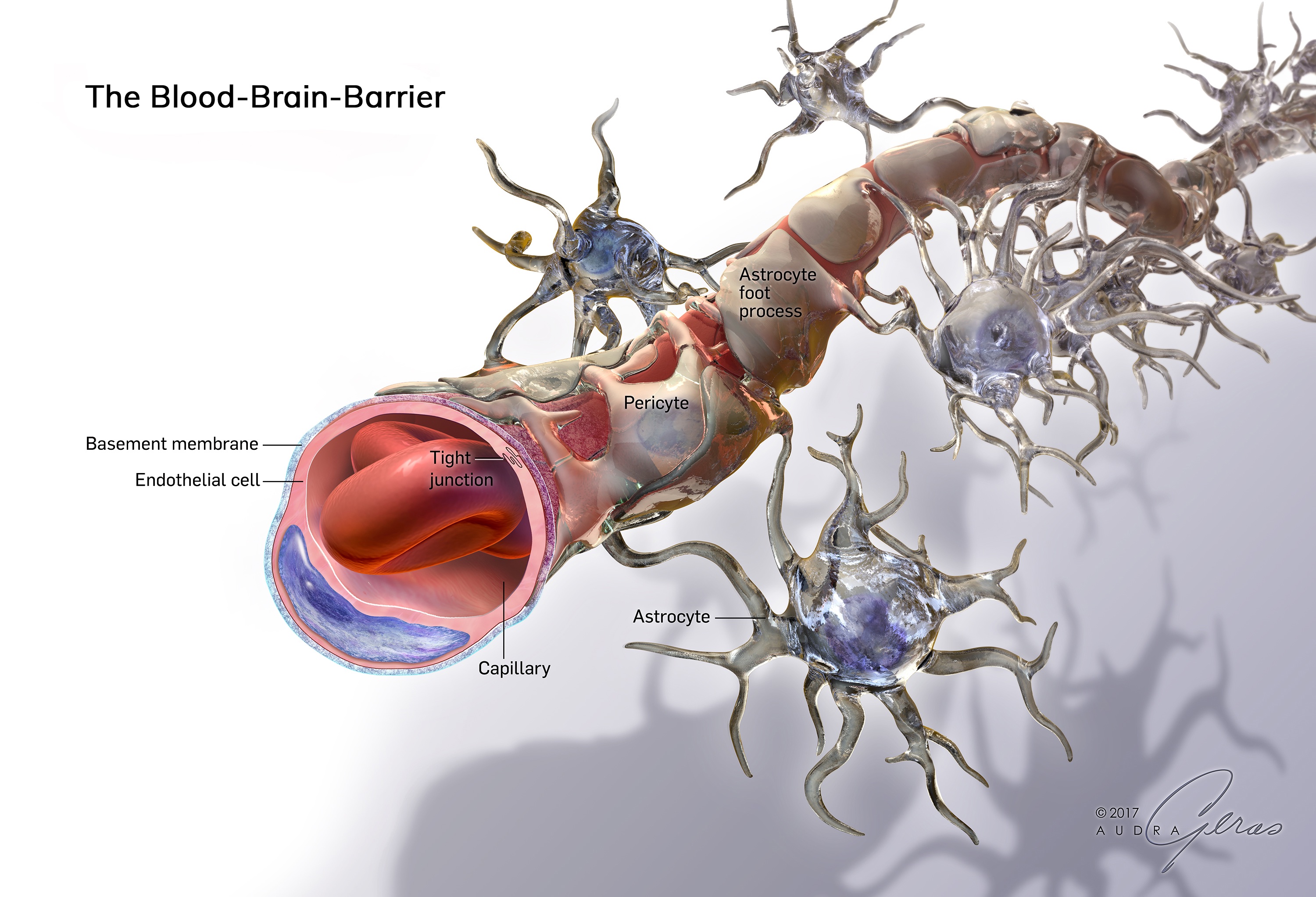
This miraculous system consists of the following structures: [1]
· Endothelial cells lining the inner surface of capillaries
· Pericyte cells located in the outer layer of the vessel wall
· Star-shaped astrocytic cells found in the brain’s gray matter
· The basal membrane that lines the base of the epithelial cells on the inner surface of brain blood vessels, separating them from the underlying connective tissue and also enveloping nerve cells
· The choroid plexus, which produces the cerebrospinal fluid surrounding the brain and spinal cord
· The pia mater and arachnoid membrane, which form the inner two layers of the three-layered membrane surrounding the brain
This barrier is critically important for the normal functioning of the brain. If the barrier is disrupted for any reason, neural inflammation begins and leads to brain cell damage. Damage to the barrier and the resulting increase in permeability may lead to the development of brain edema. The blood–brain barrier may also be disrupted in conditions such as severe starvation, liver failure, central nervous system infections, sepsis, intracranial masses, and trauma. [2]
When the physical structure or function of the blood–brain barrier is compromised, the likelihood of various central nervous system diseases increases, and problems in the barrier can cause severe systemic disorders. For example, impairments in the blood–brain barrier are thought to contribute to the development of serious central nervous system disorders such as stroke, epilepsy, meningitis, Alzheimer’s disease, and multiple sclerosis. These conditions are believed to result from disruptions in some of the tightly connected structures within the barrier.
The blood–brain barrier is created in such a highly specialized manner that, through controls made within milliseconds, it prevents toxins and harmful substances from entering while meticulously allowing the passage of nutrients necessary for brain function.
At the outer boundaries of the brain (periventricular organs), the blood–brain barrier is absent. Hormones and enzymes secreted from these regions can rapidly enter the bloodstream due to the lack of a barrier. If a barrier were present in these regions, the passage of these hormones would be impaired, and the balance necessary for maintaining healthy life would be disrupted.
STRUCTURE OF THE BLOOD–BRAIN BARRIER
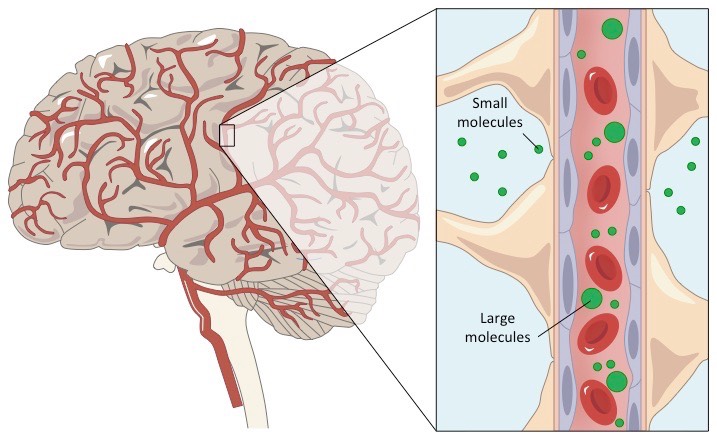
The blood–brain barrier consists of complex cellular structures created in accordance with its function in the body. Through this barrier, the passage of substances into brain cells is controlled physically by strong junctional connections and metabolically by enzymes. The capillaries of the central nervous system possess several characteristics that distinguish them from capillaries elsewhere in the body. One of these is the tight junctions between the endothelial cells lining brain capillaries and the presence of a continuous membrane (basal membrane) surrounding these capillaries.
Interestingly, there is a high electrical resistance between the endothelial cells of the blood–brain barrier. While resistance (TEER) in other tissues ranges from 3–33 Ω·cm², in the blood–brain barrier it rises to 1500–2000 Ω·cm². This electrical field creates an obstacle to the transport of fluids and ions into and out of cells, thereby reducing permeability. Moreover, unlike other capillaries in the body, the blood–brain barrier does not contain pores or gaps that would allow the passage of substances with a molecular weight below 10,000 g/mol. [3]
The barrier is also critically important in maintaining the balance of brain cells. It protects the brain from fluctuations in the blood and selectively permits the passage of necessary substances while blocking harmful ones, thereby providing the most suitable functional environment for brain and nerve cells.
The ability of many beneficial and essential substances to pass through the blood–brain barrier and enter the brain depends on a number of factors. The molecular weight of the substance, its ability to alter its three-dimensional structure, enzymatic stability within the cell, cell-derived secretions, attraction to electrical currents, hydrogen bonding potential, affinity for transporters, and the effects of existing pathological conditions are among the primary factors determining whether it receives “permission” to pass through the barrier. Less influential factors include the proportion of enzymes in the system, the capacity of plasma carrier proteins to perform binding functions, and cerebral blood flow.
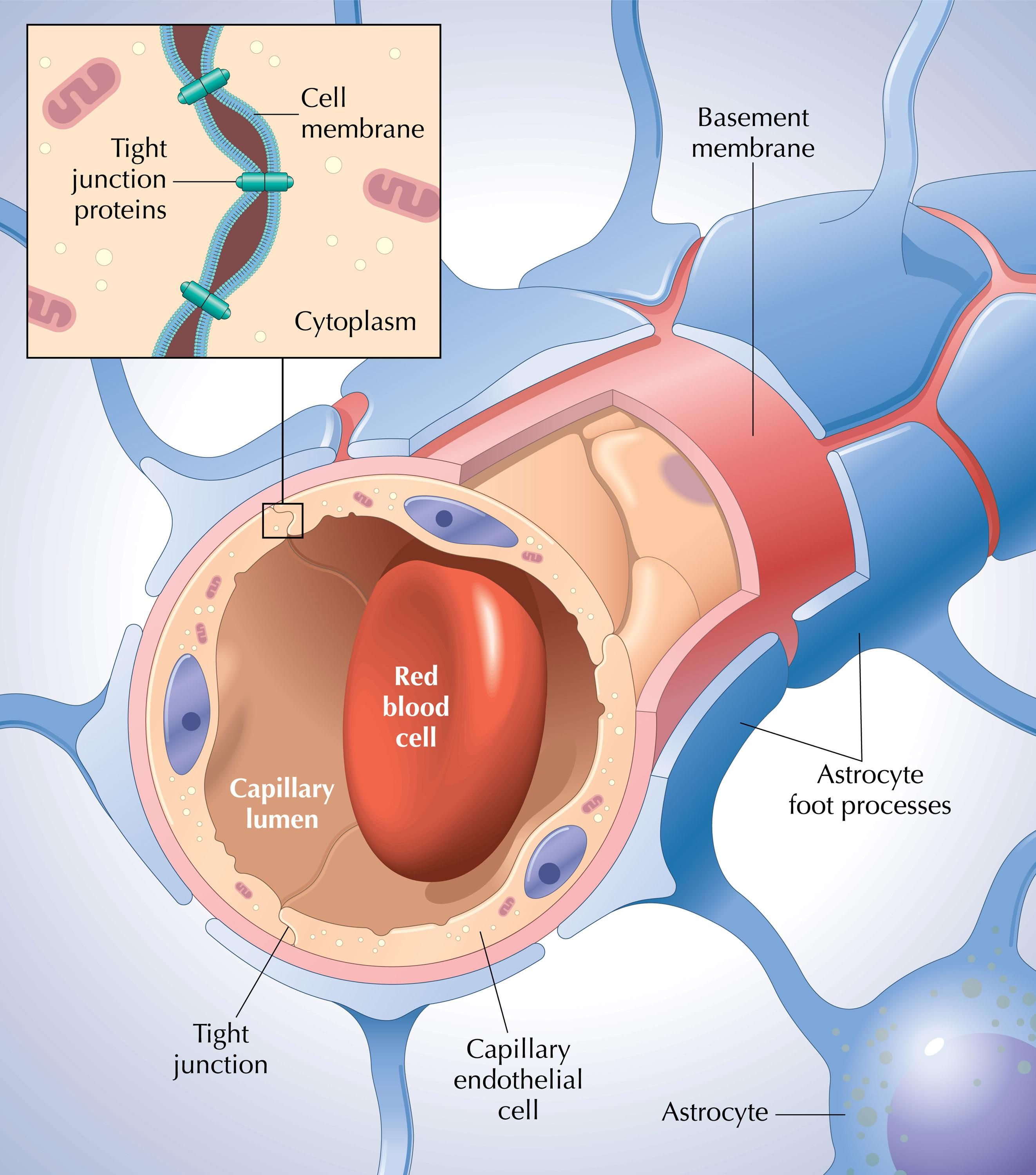
In general, transport systems that carry substances into the brain face the inner side of the blood–brain barrier, while systems responsible for transporting substances from the brain to the blood face the outer side. The transport of essential substances across the blood–brain barrier occurs through simple diffusion, facilitated transport, energy-dependent active transport, and vesicular transport. Lipid solubility, transport capacity, molecular weight, and charge are important determinants in substance transport.
The barrier also limits the rate at which certain therapeutic agents reach the brain. However, by allowing the passage of some antibiotics such as streptomycin, gentamicin, and erythromycin, it prevents the treatment of nervous system infections from becoming impossible. [4] Additionally, by permitting the passage of anesthetic agents, it makes it possible to anesthetize patients before surgical procedures.
Glucose and oxygen, which the brain requires, are privileged. They easily cross the blood–brain barrier and enter cells without obstruction. Carbon dioxide, a byproduct of metabolism, is also rapidly expelled without being hindered by this barrier. Without this extraordinary system—of which we are completely unaware—the brain would swell due to the inability to eliminate carbon dioxide or die from lack of glucose.
The blood–brain barrier is a remarkable system created both to nourish and protect the brain. Due to its complex physical and chemical properties, this system demonstrates that the human body could not have formed through random changes over time. Even a minor disruption in the barrier leads to serious diseases, and although each individual component of this multi-factor system may be present, if the system as a whole is not fully functional, it becomes impossible for a human being to live in a healthy manner.
Human beings are often unaware that such a perfect system operates within their own bodies. Yet this unnoticed system protects them from conditions that would lead to certain death. It is evident that the One Who brought the blood–brain barrier into existence, Who created the entire human body, is the Supreme Creator possessing superior knowledge and power. That Creator is our Almighty Lord, Who created the human being from a drop of fluid.
The fact that some people fail to recognize this reality demonstrates how appropriate the reminders of God are:
“We created you so why do you not confirm the truth?” (Surat Al-Waqi‘a, 57)
“It is He Who has created hearing, sight and hearts for you. What little thanks you show!” (Surat Al-Mu’minun, 78)
Sources:
[1] Ballabh P., Braun A., Nedergaard M. (June 2004). “The blood–brain barrier: an overview: structure, regulation, and clinical implications.” Neurobiology of Disease, 16(1): 1–13. doi:10.1016/j.nbd.2003.12.016. PMID: 15207256.
[2] Haluska M., Anthony M.L. (2004). “Osmotic blood–brain barrier modification for the treatment of malignant brain tumors.” Clinical Journal of Oncology Nursing, 8: 263–267.
[3] Gültürk S., et al. (2007). “Kan-Beyin Bariyeri [The Blood–Brain Barrier].” Erciyes Tıp Dergisi (Erciyes Medical Journal), 29(2): 148.
https://jcpres.com/storage/upload/pdfs/EMJ_29_2_147_154.pdf
[4] Şanlı Y., Kaya S. (1994). Veteriner Farmakoloji ve İlaçla Sağıtım Seçenekleri [Veterinary Pharmacology and Drug Treatment Options]. Ankara: Medisan Publishing House, pp. 571–650.


